
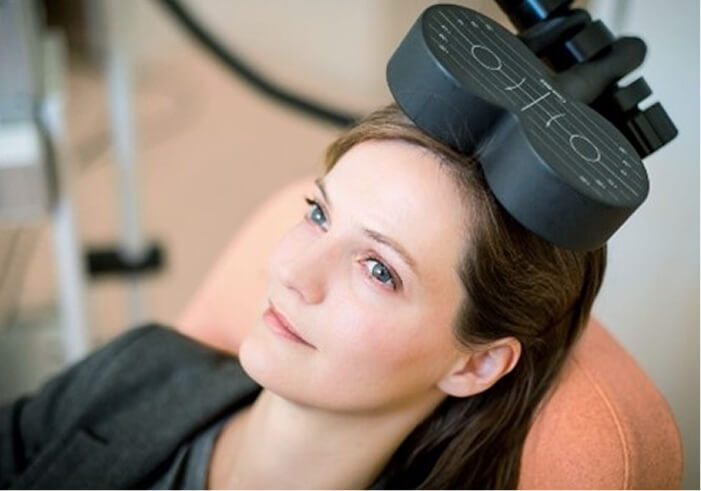
What is Transcranial Magnetic Stimulation?
Transcranial Magnetic Stimulation (TMS) is a non‑invasive brain stimulation treatment used to treat depression.
It uses targeted magnetic pulses to stimulate areas of the brain involved in mood regulation.
TMS does not involve surgery or sedation and you remain awake during treatment.
Sessions are delivered over several weeks with most people returning to normal activities straight after.
How does TMS work?
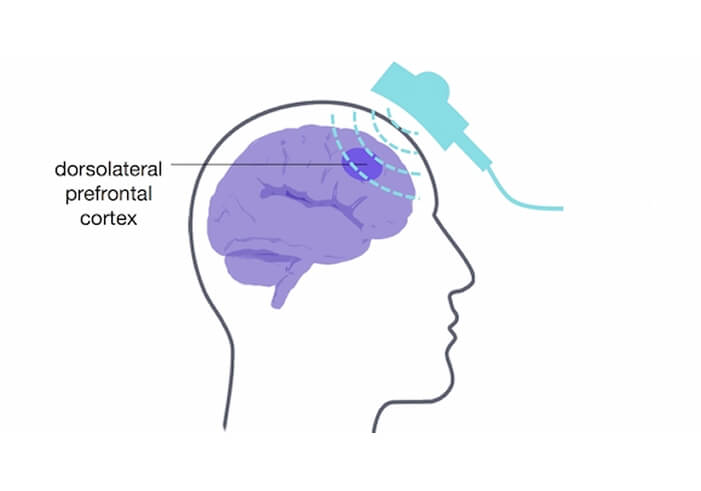
TMS most commonly targets the prefrontal cortex of the brain, a region involved in mood regulation, decision‑making and emotional control.
A small magnetic coil is placed near the scalp during treatment.
The coil delivers brief magnetic pulses to targeted areas of the brain linked to depression. Over time, this repeated stimulation may help improve communication within brain circuits involved in mood and motivation.
Each session typically lasts 20–40 minutes.
What conditions does TMS treat?
TMS is most commonly used to treat:
- Major depressive disorder
- Treatment‑resistant depression
It may be considered when antidepressant medications or therapy alone have not been effective or are difficult to tolerate.

Who is TMS for?
TMS may be suitable for adults who:
- Are experiencing ongoing depression
- Have tried antidepressant medication with limited benefit
- Are seeking a non drug, non invasive treatment option
- Can attend regular outpatient sessions
An assessment with a psychiatrist can help determine whether TMS may be a suitable treatment option for you.
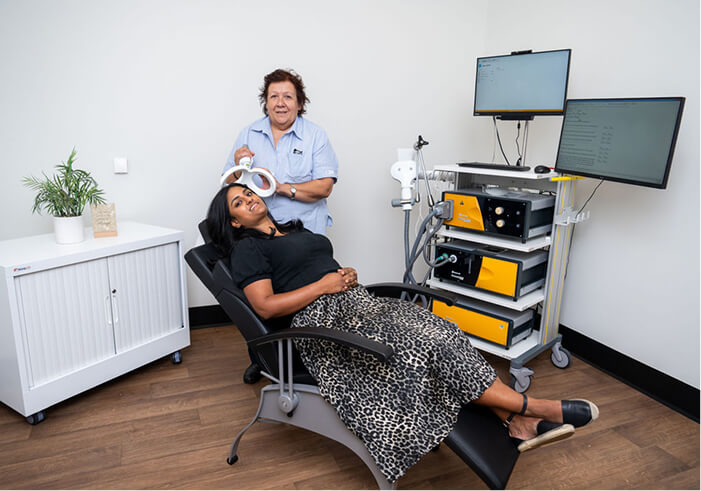
How is TMS delivered?
TMS is provided as an outpatient treatment with no hospital stay required.
Sessions take place in a private room where you sit comfortably in a chair and can relax, watch TV or listen to music during treatment.
Following treatment, you are able to head home the same day and get back to your normal daily activities.
Funding options
![]()
Private Health
In most cases, private health insurance does not cover outpatient TMS treatment. A small number of health funds may contribute in specific circumstances but prior approval and supporting medical documentation is required.
![]()
Self-funding
Self‑funded options are available for those who don’t meet Medicare criteria. Full costs will be outlined before treatment commences.
![]()
Medicare‑funded TMS therapy
Medicare rebates may be available for eligible adults with treatment‑resistant major depression who:
- Are 18 years of age or older
- Have tried at least two antidepressant medications
- Have not previously received TMS
- Meet clinical eligibility criteria following psychiatric assessment
Our team can explain eligibility and next steps as part of your enquiry.

How to access treatment
To access TMS therapy, you’ll need a referral from your GP or psychiatrist. Our team can help guide you through the next steps and confirm whether TMS may be suitable based on your needs and treatment history.
Take the next step
Contact our friendly team to see if TMS treatment may be suitable for you
Phone: (02) 9686 0700
Monday to Friday 8am to 5pm

Frequently Asked Questions
Based on current evidence, the magnetic fields used in TMS are considered safe.
This isn’t done during the initial course of TMS.
Some patients having maintenance TMS will have two sessions per day but this isn’t always the case.
This is quite variable. Generally patients can hope to see some improvement in their mood during the second or third week of treatment if TMS is going to work for them. For some patients, a response can be more delayed.
Windsor Road Private Clinic only offers TMS as an outpatient treatment only.
This means you don’t stay in hospital overnight - you come in for your TMS session and go home the same day.
We do not offer TMS therapy as part of an inpatient admission.
Those people who are going to respond to TMS usually show some initial improvement in their mood after four to six sessions.
It may take up to 20 sessions for your mood to return to its usual level.
As TMS involves magnetic energy, some people may be unable to have TMS including those with:
- A cardiac pacemaker or defibrillator
- A neurostimulator or biostimulator
- Brain aneurysm clips
- Cochlear implants
- History of previous head or brain surgery
- History of seizures, fits, epilepsy or stroke
- Or a significant neurological disorder (e.g. MS, cerebral lupus, brain tumour, etc.)
- TMS is not recommended for people during pregnancy.
People with dental fillings / braces are able to receive TMS.
You will be asked to complete and sign a safety checklist prior to receiving TMS.

